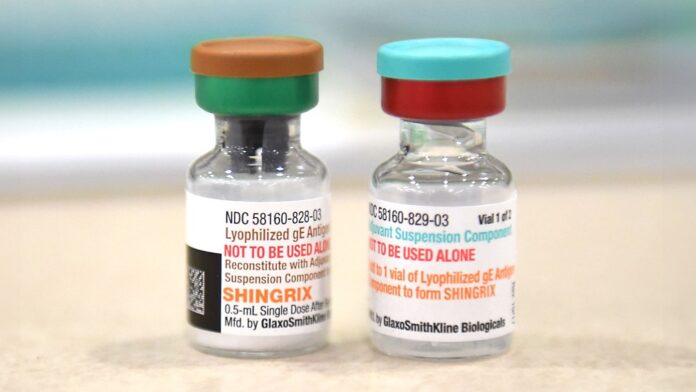
Shingles (herpes zoster) is more than just a temporary skin rash. It is a painful condition caused by the reactivation of the varicella-zoster virus —the same virus responsible for chickenpox. Once a person recovers from chickenpox, the virus remains dormant in the nervous system, potentially resurfacing decades later.
While the initial rash typically lasts about 10 days, the complications can be much more severe. Roughly 20% of patients develop postherpetic neuralgia (PHN), a condition involving debilitating nerve pain that can persist for months or even years. In some cases, shingles can even lead to vision loss or blindness.
Fortunately, modern medicine offers a highly effective way to prevent these outcomes through the Shingrix vaccine.
Who Should Prioritize Vaccination?
Because the immune system naturally weakens with age, older adults are at the highest risk. The World Health Organization (WHO) and other health authorities suggest specific groups should seek vaccination:
- Adults aged 50 and older: This is the primary target group, regardless of whether they have had shingles before.
- Immunocompromised adults (18+): Those with weakened immune systems due to conditions like HIV or cancer, or those taking specific medications, are also at high risk.
- Previous vaccine recipients: If you previously received the older live vaccine (Zostavax ), you should still get the new recombinant vaccine (Shingrix ) for better protection.
Note: If you are under 50, a doctor’s prescription is required to receive the vaccine.
Understanding the Vaccine: Effectiveness and Safety
The current standard, Shingrix, is a recombinant vaccine. Unlike the discontinued Zostavax, which used a weakened live virus, Shingrix uses only specific pieces of the virus. This means it cannot cause shingles in the vast majority of people.
How well does it work?
Research indicates that Shingrix provides robust, long-term protection:
– Ages 50–69: 97% effective at preventing shingles.
– Ages 70+: 91% effective at preventing shingles.
– Pain Prevention: Even in “breakthrough” cases where a person still develops shingles, the vaccine is highly effective (89%–91%) at preventing the dreaded long-term nerve pain (PHN).
Side Effects and Safety
While safe, the vaccine can trigger an immune response. Common side effects include:
– Soreness, redness, or swelling at the injection site.
– Fatigue, headache, or muscle aches.
– Fever, chills, or nausea.
These symptoms are generally mild and typically resolve within one to three days. In extremely rare instances, a serious neurological disorder known as Guillain-Barré syndrome (GBS) has been reported, though the risk of GBS is significantly higher from a natural shingles infection than from the vaccine.
Logistics: Cost, Coverage, and Administration
To ensure full protection, Shingrix requires a two-dose series. The second dose should be administered two to six months after the first (or one month later for those with weakened immune systems).
Is it affordable?
In the United States, financial barriers are minimal for most:
– Insurance Coverage: Under the Affordable Care Act (ACA), most private insurance, Medicaid, and Medicare Part D cover the vaccine at no out-of-pocket cost.
– Uninsured Patients: Those without coverage may need to pay out of pocket or apply for manufacturer assistance programs. The estimated cost is approximately $234.69 per dose.
Where to go?
The vaccine is widely available at most pharmacies. For many, an appointment is required, but a doctor’s prescription is not necessary if you meet the age or health eligibility criteria.
Summary: Shingles can cause lifelong nerve pain, but the Shingrix vaccine offers highly effective protection for adults over 50 and those with weakened immune systems. Most patients can access this two-dose series at no cost through their insurance providers.